Article

Effective August 31, 2017, Ohio’s health care regulatory boards implemented new limits on prescriptions issued for the treatment of acute pain. The rules in Ohio’s opioid law are only intended to treat conditions resulting in acute pain, including those that normally fade with healing such as a surgical procedure or a bone fracture.
Highlights of Ohio’s opiate prescribing limits for acute pain include:
Additionally, since December 23, 2018 Ohio prescribers are required to follow regulations when prescribing opioids for the treatment of long-term pain (lasting 12 weeks or more) and subacute pain (lasting between six and 12 weeks). The specific requirements can be found in Ohio Administrative Code 4731-11, but the State Medical Board of Ohio published a condensed overview of those regulations.
According to the National Institute on Drug Abuse, in Ohio, drug overdose deaths involving opioids dropped from 4,293 in 2017 (a rate of 39.2) to 3,237 in 2018 (a rate of 29.6)
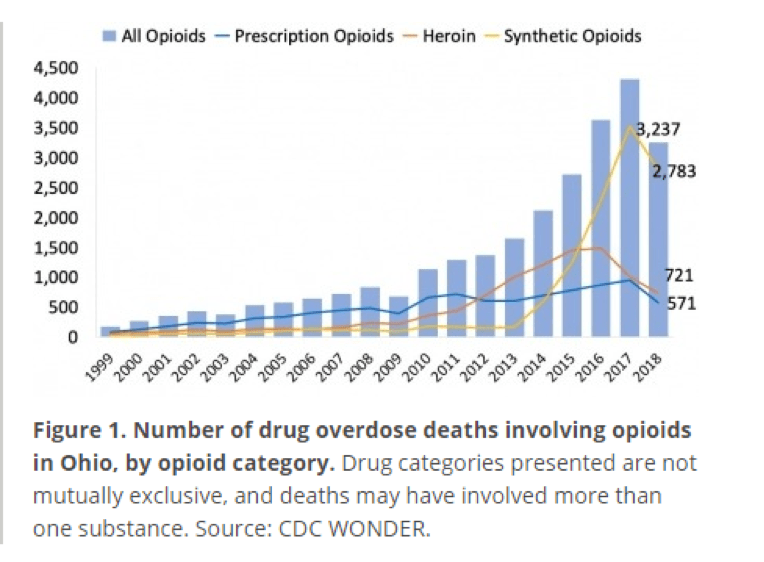
Unfortunately, according to the Ohio Attorney General, Dave Yost, in 2020 more Ohians died of an opioid overdose during a 3-month period than at any time since the opioid epidemic began. The analysis by Yost’s Scientific Committee on Opioid Prevention and Education (SCOPE) found the death rate in Ohio from an opioid overdose at 11.01 per 100,000 population in the second quarter of 2020 – the highest rate in 10 years. The previous 10-year high was in the first quarter of 2017 at 10.87 opioid overdoses per 100,000 population.
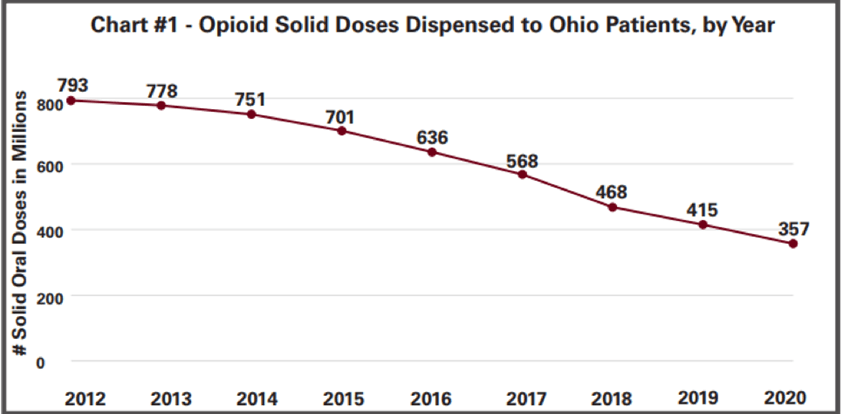
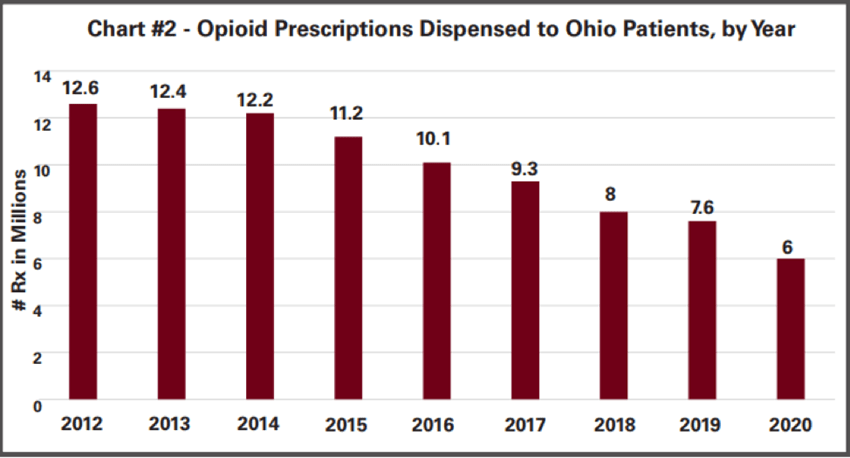
As for the prescription of opioids across the state, according to the 2020 annual OARRS report, the number of opioid doses (solid dosage units only) and prescriptions dispensed to Ohio patients in 2020 continued to decrease. Total doses of opioids decreased from a high of 793 million in 2012 to 357 million in 2020, a 55 percent decrease (Chart #1). The total number of opioid prescriptions decreased by 6.6 million between 2012 and 2020, a 52 percent decrease (Chart #2).
In order to help enforce the limited exceptions to Ohio’s opioid rules and to enhance data regarding opioid trends, prescribers in Ohio are required to include a diagnosis or procedure code on every controlled substance prescription, which then must be entered into Ohio’s prescription monitoring program, the Ohio Automated RX Reporting System (OARRS).
OARRS is a tool to track the dispensing and personal furnishing of controlled prescription drugs to patients. It is designed to monitor this information for suspected abuse or diversion (i.e., channeling drugs into illegal use), and can give a prescriber or pharmacist critical information regarding a patient’s controlled substance prescription history.
The OARRS website also contains a lot of helpful documents and resources for Ohio prescribers to familiarize themselves with.
We encourage providers regardless of state, law, rule or medical guidelines to consider the following items when prescribing opioids in the state of Ohio:
These monitoring activities, as well as others, should always be combined with the provider’s thorough assessment of the patient in order to achieve the best outcomes.
When it comes to protecting patient health and covering yourself from liability, utilizing toxicology screening is essential. Of the five best practices listed above, toxicology is the most objective and scientific way to detect and prevent opioid misuse. Toxicology screening shows what the patient actually ingested and what is actually in their body.
With expertise in toxicology screening, DRUGSCAN’s Prescription Drug Monitoring services take a proactive approach to patient safety by providing valuable information to providers regarding patient medication use. Early detection of medication misuse allows for early intervention and better patient outcomes. From providers in large institutions to smaller private audiences, we provide the tools necessary to responsibly prescribe and monitor the use of opioids.
Whether you’re a private physician or working in medical practice within a large hospital system, DRUGSCAN offers testing services that help you make critical decisions regarding your patients, quickly and efficiently.
Contact us to learn about our suite of toxicology services, including Prescription Drug Monitoring.